Abstract
Objectives
Acoustic rhinometry is a rapid, reliable and non-invasive technique for the evaluation of conditions associated with impaired nasal patency. This study aimed to examine the intersession repeatability of acoustic rhinometry measurements of unilateral and combined nasal parameters in a group of healthy volunteers.
Methods
Twenty healthy volunteers were studied. In each subject, acoustic rhinometry measurements were performed on five consecutive days, with multiple recordings. Five clinically relevant parameters were measured in each session and the intersession repeatability of these measurements was expressed in terms of mean coefficient of variation, intraclass correlation coefficient and inter-item correlations.
Results
Intraclass correlation coefficients showed a high, and greater repeatability over time for all the combined (mean) values compared to the unilateral values. All intraclass correlations for combined values were ≥0.80 confirming almost perfect agreement. All intraclass correlations and inter-item correlations were associated with P<0.001. The mean coefficient of variation was low (<10%) for all but the proximal minimum cross sectional area (MCA1) measurements.
Conclusion
Acoustic rhinometry provides highly repeatable measurements of nasal patency, which is best for combined (mean) nasal parameters. This property makes it suitable for use in the diagnosis and follow-up of conditions associated with nasal obstruction, either structural or functional.
INTRODUCTION
The clinical use of acoustic rhinometry was first described by Hilberg et al. [1] in 1989 as an objective method to examine the patency of the nasal cavity. It estimates intranasal volume between predefined segments, and cross-sectional areas through identification of local changes in acoustic impedance using a sound pulse propagating in the nasal cavity. Since nasal obstruction is common in a wide range of sinonasal disorders, the technique may have an important role in the diagnosis and follow-up of conditions altering intranasal dimensions, either permanently or transiently.
Since its introduction, acoustic rhinometry has been investigated and used in many conditions in adults and children including allergic rhinitis, vasomotor rhinitis, nasal, pharyngeal and maxillofacial procedures and conditions, and sleep disorders [2]. Acoustic rhinometry is not only able to detect irreversible structural changes but also reversible dynamic changes, providing information on both the location and reversibility of the pathological condition.
Correlation and/or agreement of the technique with other diagnostic methods including rhinomanometry, computed tomography, optical rhinometry, magnetic resonance imaging, direct X-ray examination, fiberoptic nasal endoscopy and clinical findings has been well established in both clinical and experimental settings [3-11], although acoustic rhinometry seems to have some limitations in the posterior part of the nose [9, 12, 13] and interchangeable use of different methods is not appropriate [14].
The automated nature of the technique and dependency of measurements on position necessitates the confirmation of its repeatability in serial measurements over consecutive sessions. The intersession repeatability of acoustic rhinometry remains to be clarified and this has important clinical implications, particularly when the method is to be used for the purpose of follow-up. No previous study has examined the intersession repeatability of acoustic rhinometry using the gold-standard intraclass correlation coefficient, comparing combined (mean) and individual nares, in healthy subjects [15-20]. We designed a study to assess this.
MATERIALS AND METHODS
Subjects
Twenty healthy subjects (13 males, 7 females) without a history of nasal symptoms or disease were included in this study. The mean (SD) age of the subjects was 38±7.11 years. None of the subjects were on nasal medications. All subjects provided informed consent prior to study entry. The study received ethics approval from the Royal Free Hampstead Trust ethics committee (study reference is 09/H0720/24).
Measurement technique
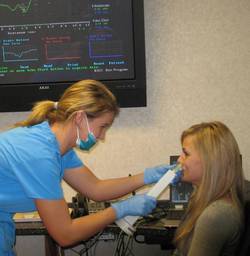
Acoustic rhinometry measurements were performed in accordance with a previously published protocol [21]. The acoustic rhinometry device was A1 acoustic equipment with an updated software ver. 0.5 (GM Instruments, Kilwinning, UK). Measurements were obtained when the subject was in a sitting position and under close supervision of the operator. Each subject was instructed to open the mouth and stop breathing during the measurements. The sound tube was handheld by the subject to obtain a sealed nostril. Fig. 1 shows the handling and positioning of the wave tube by the subject. All measurements were obtained by the same operator in the same air-conditioned room to provide similar conditions with regard to temperature, humidity and ambient noise level. Multiple recordings were taken for each subject at each visit and curves with obvious artefact were discarded. For each subject, measurements were repeated on five consecutive days.
Variables
Five important acoustic rhinometry variables were assessed and examined separately to test the intersession repeatability of the technique: outermost minimum cross-sectional area (MCA1, cm2), the distance of MCA1 from the nasal orifice (D-MCA1, cm), innermost minimum cross-sectional area (MCA2, cm2), the distance of MCA2 from the nasal orifice (D-MCA2, cm), and the volume of the nasal segment between the 2nd and 5th cm from the nasal orifice (V2-5, cm3). MCA1 corresponds to the level of nasal valve, whereas MCA2 corresponds to the anterior half of inferior turbinate. In each subject on each day, areas, distances and volume values for each separate nostril were averaged (mean), whereas combined values were obtained by calculating the mean of the mean results from the right and left nostrils to correct for the variation between nostrils during the nasal cycle. Fig. 2 illustrates a typical rhinometry trace from one of the subjects.
Statistical analysis
SPSS ver. 18.0 (IBM, New York, NY, USA) was used for the analysis of data. Intraclass correlation coefficients were used to examine intersession repeatability of each parameter measured over five separate occasions for unilateral and total (combined right and left) values. Intraclass correlation coefficient values were interpreted as follows: 0.41-0.60, moderate agreement; 0.61-0.80, substantial agreement; >0.80, almost perfect agreement [22]. In addition, the mean coefficient of variance and inter-item correlations were calculated for each parameter. A P-value<0.05 was considered indicative of statistical significance.
RESULTS
Table 1 reports the repeatability estimates of combined (mean of left and right) values for the five different acoustic rhinometry measurements. Intraclass correlation coefficients and inter-item correlation coefficients indicated excellent agreement for all parameters across five separate sessions. All intraclass correlations were ≥0.80 confirming almost perfect agreement. All intraclass correlations and inter-item correlations were associated with P-values<0.001. The mean coefficient of variation was low (<10%) for all but MCA1 measurements (14.5%). The coefficient of variation was particularly low for D-MCA1 (7.4%), D-MCA2 (2.8%), and nasal volume (5.4%). Unilateral data from the right and left nostrils are also presented in Table 1. Agreement was less good (lower intraclass correlation) than when using data from both nostrils combined.
DISCUSSION
This is the first study to examine the intersession repeatability of acoustic rhinometry using intraclass correlation coefficients on averaged combined, and separate nostril minimum cross-sectional areas and nasal volumes. We showed that acoustic rhinometry provides excellent reproducible results, best over different sessions when combined nasal parameters values are used than right or left nostrils separately. This degree of repeatability has clinical implications with regard to the utilization of this rapid and easy-to-use technique in the follow-up of conditions associated with impaired nasal patency.
The measurements obtained in this study included a wide range of clinically relevant parameters: minimum cross-sectional area at two distinct points and their corresponding distances from the nostrils, and the volume of the nasal cavity between the 2nd and 5th cm. The MCA1 corresponds to the nasal valve and is a good indicator of structural obstruction, whereas the MCA2 corresponds to the anterior half of the inferior turbinate, which contains erectile tissue and therefore is a reflection of functional obstruction. Similarly, the region of the nasal cavity between the 2nd and 5th cm is the site of mucosal changes; thus this volume is also considered a reflection of functional obstruction.
To date, several studies have examined the intersession repeatability of acoustic rhinometry measurements in both healthy individuals and in patients with nasal obstruction, but each has limitations, which we have attempted to address in the present study design. Similar to the current study, except not using combined values for nostrils, Silkoff et al. [18] examined the repeatability of acoustic rhinometry measurements performed on five separate occasions and found relatively low variation in minimal cross-sectional area and nasal volume (0-5 cm). Measurements of minimal cross-sectional area showed 8.1% and 9.7% variation for the right and left sides, whereas variations were even lower for nasal volumes (4.8% and 5.5%, respectively). Intraclass coefficients for right and left MCA were 0.91 and 0.87, whereas corresponding figures for nasal volume were 0.86 and 0.69, respectively. This study, unlike ours, did not combine values from both nostrils and therefore does not account for variation with nasal cycle. We showed that combined results were more repeatable than those from individual nostrils. In a separate study, Castano et al. [15] examined the repeatability of acoustic rhinometry measurements in patients with occupational rhinitis and found low variation in both minimal cross-sectional area and nasal volume measurements. Intersession intraclass correlation coefficients ranged from 0.80 to 0.88 and from 0.83 to 0.94 for nasal volume and MCA, respectively. These figures are in agreement with the findings of this study on healthy individuals.
Harar et al. [16] investigated the repeatability of acoustic rhinometry measurements on day-to-day basis using the minimal cross-sectional area at the nasal valve level (MCA1). They made measurements on two separate days and found a relatively high mean intersession difference (12.9%) when only one measurement was performed at each visit and this mean intersession difference could only be reduced to 10.85% when ten recordings were done for each subject at each visit. We also report a higher variation in minimal cross-sectional area measurements at the nasal valve; however, intraclass correlations calculated using measurements on five consecutive days showed better agreement. The high variation in MCA1 measurements (14.5%) may possibly be attributed to the malpositioning of the device by the patient. However, intraclass correlation takes into account correlations between every pair of observation and thus may be regarded as a more accurate means for examining the repeatability of the measurements over time. Similarly, Ognibene et al. [17] found relatively low agreement between measurements obtained on two different sessions one week apart, with intraclass coefficient of 0.67. The high intraclass correlation coefficients obtained in the present study may be attributed to the relatively short duration between measurements in contrast to the Ognibene study [17], which may cause bias due to carry-over effect. However, we believe that normal mucosal variations, even in normal subjects, would also bias against better repeatability if the duration between measurements were longer.
Most previous studies have assessed parameters for the individual nasal cavity (either right or left) separately; however, in our study we used combined (mean) parameters from the two nostrils to correct for the variations between nostrils during the nasal cycle. This may also account for the almost perfect agreements found in this study. Similarly, Roithmann et al. [19] found less intersession coefficient variation for combined parameters when compared to unilateral parameters, but this paper does not report the gold standard assessment of intraclass correlation.
Acoustic rhinometry is a rapid, convenient and reliable technique to examine nasal patency. Although there are several techniques that can be utilized for this purpose, acoustic rhinometry has several advantages. The benefits of rhinomanometry have been demonstrated in many clinical settings; however, it does not give an idea on the localization of the obstruction. Nasal endoscopy on the other hand is not able to produce quantitative results, although it provides excellent visual topography. Similarly, nasal examination provides only subjective information on the degree of obstruction. Acoustic rhinometry has the ability to localize and quantify both reversible and irreversible obstruction of the nasal cavity. However, since it is a position dependent procedure, concerns related to the repeatability of measurements have arisen. Current evidence suggests that repeated measurements should be made in each session to obtain a reasonable level of reproducibility [23]. In addition, Harar et al. [16] reported better intersession repeatability when multiple measurements were done in each session. Intersession repeatability itself is important particularly when the technique is to be used for follow-up purposes. Therefore, multiple recordings were made in each session of this study to avoid the effects of intra-session variability.
The accuracy of acoustic rhinometry has shown to be higher for the anterior part of the nose when compared to posterior part [9, 12, 13]. Tarhan et al. [13] reported that acoustic rhinometry overestimates cross-sectional area beyond paranasal sinus ostia. In this study, both minimal cross-sectional areas measured at two different levels showed similar repeatability, suggesting that acoustic rhinometry provides reproducible results at as far as the level of anterior half of the inferior turbinate.
In conclusion, using intraclass correlations in healthy subjects, combined acoustic rhinometry measurements (mean of left and right nostrils) provide excellent and more reproducible estimates of nasal geometry over time than assessing each nostril separately, in terms of both localization and reversibility of pathological obstructions, supporting its use for the follow-up of conditions associated with structural or functional obstruction.



